(March 12, 2026) — Texas Biomedical Research Institute is studying and innovating new tools – known as new approach methodologies (NAMs) – that can accelerate discoveries and drug development by complementing required studies to ensure new medicines are safe for people.
NAMs are tools, such as AI-based computer modeling, advanced cell culture and complex microphysiological systems, that aim to study disease and test treatments using human-relevant biology. Currently, nonhuman primates are the gold standard model for evaluating and predicting how humans will react to a new medicine, therapy or vaccine. Texas Biomed’s Southwest National Primate Research Center (SNPRC) is one of seven federally supported National Primate Research Centers with decades of experience in the complex process of establishing, refining and testing such model systems. These centers are also applying that same scientific rigor and specialization to establish biological standards for NAMs to ensure reliability and safety for potential future human applications.
“We all love animals and our goal is to get to a day when we don’t need them to help understand complex biological systems and assess if treatments and medicines are safe and effective before being tested in people,” said SNPRC Director Corinna Ross, PhD. “While that day is still many years away, we are actively working to progress science towards that goal.”
3Rs: Replace, reduce and refine
As a nationally recognized leader in nonhuman primate care and research, SNPRC follows the 3Rs: replace, reduce and refine. Researchers use additional tools, including NAMs, whenever possible to replace the need for animal research to answer critical questions; they are required to reduce animal numbers to the absolute minimum needed for scientifically rigorous studies; and teams constantly seek ways to refine studies for the health and welfare of animals.
“Every animal is a precious resource and so every study is reviewed and monitored by multiple oversight teams from proposal through implementation,” said Eric Vallender, PhD, SNPRC Associate Director of Research. “As much as possible, we look for alternatives to nonhuman primates. When cell or computational models aren’t appropriate and other animal models won’t work, we first direct investigators to banked tissue samples or look for ways to piggyback on other studies. Always, always, always, we only allow the smallest number of animals that are needed to provide trustworthy results.”
NAMs have been under development for decades
Credit: iStock
NAMs that can speed up drug discovery and screenings and thereby help reduce the overall number of animals needed in early phases of preclinical testing have been under development for decades.
For example, organoids are 3D cellular structures that are simplified, miniature representations of individual tissues or organs, such as lung, liver, heart and brain. Organ-on-a-chip systems – also called microphysiological systems (MPS) – are devices that aim to mimic dynamics within tissues, including cell interactions and flowing fluids. Machine learning and artificial intelligence promises to help model and predict potential treatment targets, drug compounds and interactions.
In the last few years, the federal government has introduced legislation, proposed a roadmap and launched research funding challenges aimed at accelerating NAM development and incorporating them as part of the formal safety and efficacy studies of new drugs required for approval by the U.S. Food and Drug Administration (FDA).
NAMs progress and misconceptions

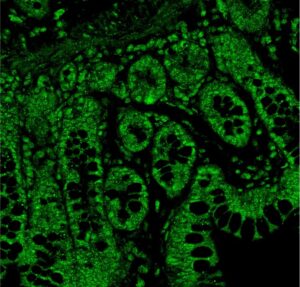
For many years, Texas Biomed and SNPRC have been collaborating with researchers across the nation on NAM development for a wide range of diseases using tissue samples. This includes brain organoids for studying epilepsy; intestinal organoids for testing antivirals; and placental organoids to understand fetal development.
Texas Biomed and SNPRC teams are also beginning development of organoids and MPSs for studying deadly pathogens like Ebola virus and therapies and vaccines that can protect against them. They are particularly focusing on how nonhuman primate organoids and tissues can support this work, combining deep expertise in nonhuman primates and high-containment research.
“There are two major misconceptions about NAMs that I’d like to help dispel,” said Texas Biomed President/CEO Larry Schlesinger, MD. “One is that they are ready to completely replace animal studies today – they are not. The second is that people tend to associate organoids and MPS with human cells and tissues, when I feel that there is significant value in developing nonhuman primate organoids as well.”
Comparing NAMs and whole model systems
The nonhuman primates at Texas Biomed and SNPRC are extremely well characterized, meaning researchers have spent many years to learn a great deal about their genetic history, physiology and immunology, which is very similar to humans. They also have determined which species are most helpful to study different diseases and test new therapies and vaccines that benefit human health.
For example, SNPRC is home to the largest marmoset colony in the U.S., which supports studies into aging, cognitive decline, Alzheimer’s disease, obesity and reproduction; macaques, which support studies of HIV, tuberculosis, COVID-19 and other respiratory infections; and the largest pedigreed baboon colony in the U.S., with genetic history going back eight generations. Baboons are especially helpful in studying nutrition, heart disease, diabetes and other metabolic conditions that affect susceptibility to disease.
“Our detailed understanding of our colonies means that we can establish organoids and MPS based on our nonhuman primates that will enable really strong studies to see how they perform compared to the whole animal,” said Dr. Vallender. “This allows us to determine with confidence how and when these new tools can be incorporated into studying human health and disease. We’ll be able to show when they work well and when more development is needed.”
Ensuring new tools are accurate and safe
Specifically, the team plans to develop systems to replicate nonhuman primate lung, airways, skin, mucus membranes and the blood-brain barrier, which like in humans, provides a protective barrier to prevent harmful particles entering the brain, but also keeps out medicines that could be beneficial. Once developed, researchers would be able to first see how a pathogen or drug behaves in the isolated, miniaturized organ systems compared to an entire animal. Such comparison studies are vital – and required by federal regulators – to see how these new tools can be used to help test the safety and efficacy of new medicines, therapies and vaccines before they are tested in people.
“As NAMs are developed, it is imperative to check that they are accurate and replicate the same results seen in the body,” Dr. Vallender said. “Nonhuman primates will play an important role in helping develop these new technologies and advance the entire field. As much promise as these NAMs offer, this step is critical before we can be confident about relying on them to assure safety in humans.”
SNPRC houses a massive repository built over 20 years of cryopreserved tissues with thousands of samples. The team will also investigate if the frozen material can be used to generate functional organoids for studying health and disease conditions.
New technologies at Texas Biomed
The Institute recently acquired the EMULATE organ-chip system, which is a platform for culturing and studying cells in a 3D environment that better approximates real tissues, complete with flowing fluids and nutrients. This system will enable researchers to conduct critical tests with both human and nonhuman-primate-based organoids.
A key challenge with developing human-based organoids and MPSs is getting suitable cells and blood from people. Dr. Schlesinger and members of his lab have developed a cellular culture system for generating human airway cells from immune cells found in blood. This makes it much easier to generate important cells that reside deep in the lungs, which previously were only accessed by costly and invasive procedures. The scientists are working to incorporate these “alveolar macrophage-like” cells into the EMULATE lung-chip system, which can help accelerate research into a wide range of respiratory conditions and diseases, such as influenza, tuberculosis and aging.
Complementary approach
In some cases, it will be extremely difficult to fully replace nonhuman primates in research studies. For example, how will we know if off-target side effects are detected without testing in a complete biological system? At this time, NAMs, even combined, cannot fully replicate a complete immune system.
“We are very hopeful that NAMs will be able to reduce the number of animals required for necessary safety and efficacy studies of new treatments, but we anticipate an integrated, balanced approach that combines both NAMs and animals will be the way forward so people are kept safe,” Dr. Schlesinger said.
The FDA has suggested investigating shortening the length of some toxicity studies in animals from six months to three months, if other data indicates toxicity is likely to be low – something industry has also proposed. Specifically, the FDA suggested trying this first with monoclonal antibodies, which are already known to have low toxicity. But the agency also stressed that side-by-side evaluations will be needed to feel confident the shorter process is sufficient to protect consumers.
“We have an incredible team of over 150 people who work tirelessly every day to ensure our animals receive the very best care,” Dr. Schlesinger said. “We are proud to set the highest bar in animal welfare, advance tools to help reduce the number of animals needed and make the world a healthier place for all.”